- Author: Kathy Keatley Garvey

Researchers from Harvard Medical School and the University of California, Davis, blocked the progression of cancer growth caused by environmental carcinogens and food contaminants by resolving an eicosanoid/cytokine storm triggered by cell debris.
The research, from the laboratories of physician-researcher Dipak Panigrahy of Harvard Medical School and UC Davis distinguished professor Bruce Hammock, is published in the current edition of the Proceedings of the National Academy of Sciences.
“We advanced the hypothesis that cell debris from chemotherapy, resection of tumors and even immunotherapy can make these therapies a double-edged sword stimulating cancer growth and metastasis while treating it,” said Hammock, who holds a joint appointment in the UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center.
In their paper, “Resolution of Eicosanoid/Cytokine Storm Prevents Carcinogen and Inflammation-Initiated Hepatocellular Cancer Progression,” the scientists covered the potent environmental carcinogen and food contaminant aflatoxin. Aflatoxins are toxins produced by certain fungi that are found in such agricultural crops as corn, peanuts, cottonseed, and nuts.
“Not only is this fungal metabolite genotoxic but it is also a tumor promoter,” said Hammock, defining a genotoxic agent as “a chemical that damages cellular DNA, resulting in mutations or cancer.”

Lead authors Anna Fishbein of Harvard University, a recently enrolled medical student in the Georgetown University School of Medicine, and Weicang Wang, a postdoctoral scholar in the Hammock lab, said aflatoxin exerts some of its cancer-promoting effects by generating cell debris which activate a pathway leading to eicosanoid and cytokine storms. These two classes of natural chemical mediators, they explained, control many of our defenses against pathogens, but when out of control, these storms lead to growth and metastasis of liver cancer.
“We demonstrated that debris generated by aflatoxin B1accelerates tumor dormancy escape in liver cancer models by stimulating a macrophage-derived eicosanoid and cytokine storm of pro-inflammatory mediators,” said Fishbein. “Thus, targeting a single inflammatory mediator or eicosanoid pathway is unlikely to prevent carcinogen-induced tumor progression.”
The researchers showed that the inhibition of the soluble epoxide hydrolase (sEH) pathway or the combined inhibition sEH and cyclooxygenase-2 (COX-2) pathways prevented the carcinogen debris-induced storm of both cytokines and lipid mediators by macrophages--specialized detect-and-destroy cells.
In animal models, the dual COX-2/sEH inhibitor PTUPB prevented the onset of debris-stimulated liver cancer. The dual inhibition of COX-2/sEH pathways may be “a novel approach” to control cancer of the liver, the researchers said.

“We also showed that carcinogen-generated debris stimulates an endoplasmic reticulum (ER) stress response which may promote HCC progression. Importantly, PTUPB prevents the ER stress response,” Wang added. “We created a novel model of debris-stimulated liver cancer designed to study new strategies for the prevention and treatment of carcinogen-induced cancers with tremendous potential to translate to the clinic.”
From a nutritional standpoint, aflatoxin is a common food contaminant, Wang said. “But good agricultural practice and post-harvest technology keep the levels very low. However, in much of the world, aflatoxin levels are so high that many crops are discarded. In other cases, these contaminated grain and nut crops enter the human food chain, where they cause acute toxicity, severe anemia and of course later lead to cancer.”
UC Davis co-author and nutritional scientist Yuxin Wang (who is the wife of Weicang Wang) said that “finding a way to modulate the events that lead to the eicosanoid storm would have a major effect on children's health in many developing countries.”

Fishbein and Allison Gartung of the Panigrahy lab not only used the soluble epoxide hydrolase inhibitors from the Hammock lab but also used some prototype drugs synthesized by chemist Sung Hee Hwang of the UC Davis School of Veterinary Medicine “which proved to be even better,” Hammock said.
“These compounds are a synthetic combination of cyclooxygenase inhibitors like celebrex with epoxide hydrolase inhibitors,” Hammock said. “Since epoxide hydrolase inhibitors stabilize the endoplasmic reticulium stress response and transcriptionally down regulate inflammatory cyclooxygenase we expected them to synergize with cyclooxygenase inhibitors. We were surprised and pleased with the dramatic interaction of these inhibitors when combined in the same molecule in reducing the cytokine and eicosanoid production by in response to cell debris.”
“The observations from Harvard show that by inhibiting soluble epoxide hydrolase, we can block the activation of these inflammatory cascades leading to tumor promotion, growth and metastasis,” Hammock said. “We have a compound in human clinical trials that inhibits sEH, which should be clinically available in a few years. In addition. we have found natural inhibitors of the epoxide hydrolase in a variety of plants, including crop plants. This may allow us to reduce the cancer risk and block the gastrointestional erosion and bleeding caused by dietary aflatoxin using natural means.”
Other members of the 15-member team are UC Davis researchers Jun Yang, Yuxin Wang and Sung Hee Hwang; Harvard researchers Haixia Yang, Victoria Hallisey, Jianjun Deng, Sanne Verheul, Allison Gartung, Diane Bielenberg and Mark Kiernan (now of Bristol-Myers Squibb); and Sui Huang, Institute for Systems Biology, Seattle. Hammock and Panigrahy are the corresponding authors.
The research drew strong financial support as the Panigrahy's laboratory is generously supported by the Credit Unions Kids at Heart Team, the CJ Buckley Pediatric Brain Tumor Fund, and the Joe Andruzzi Foundation; and Hammock's UC Davis grants from the National Institute of Environmental Health (NIEHS) Superfund Research Program, and the NIEHS RIVER Award (Revolutionizing Innovative, Visionary, Environmental Health Research).
Hammock, a member of the UC Davis faculty since 1980, has directed the UC Davis Superfund Research Program for nearly four decades. It supports scores of pre- and postdoctoral scholars in interdisciplinary research in five different colleges and graduate groups on campus. Last year Hammock received a $6 million, eight-year “Outstanding Investigator” federal grant for his innovative and visionary environmental health research: The award is part of the Revolutionizing Innovative, Visionary Environmental Health Research (RIVER) Program of NIEHS.
The abstract:
“Toxic environmental carcinogens promote cancer via genotoxic and nongenotoxic pathways, but nongenetic mechanisms remain poorly characterized. Carcinogen-induced apoptosis may trigger escape from dormancy of microtumors by interfering with inflammation resolution and triggering an endoplasmic reticulum (ER) stress response. While eicosanoid and cytokine storms are well-characterized in infection and inflammation, they are poorly characterized in cancer. Here, we demonstrate that carcinogens, such as aflatoxin B1 (AFB1), induce apoptotic cell death and the resulting cell debris stimulates hepatocellular carcinoma (HCC) tumor growth via an ‘eicosanoid and cytokine storm.' AFB1-generated debris up-regulates cyclooxygenase-2 (COX-2), soluble epoxide hydrolase (sEH), ER stress-response genes including BiP, CHOP, and PDI in macrophages. Thus, selective cytokine or eicosanoid blockade is unlikely to prevent carcinogen-induced cancer progression. Pharmacological abrogation of both the COX-2 and sEH pathways by PTUPB prevented the debris-stimulated eicosanoid and cyto- kine storm, down-regulated ER stress genes, and promoted macrophage phagocytosis of debris, resulting in suppression of HCC tumor growth. Thus, inflammation resolution via dual COX-2/sEH inhibition is an approach to prevent carcinogen-induced cancer.”
- Author: Kathy Keatley Garvey


Cancer research published by a team of scientists, including the Bruce Hammock laboratory, University of California, Davis, has been named the Journal of Clinical Investigation's Editor's Pick for the month of July.
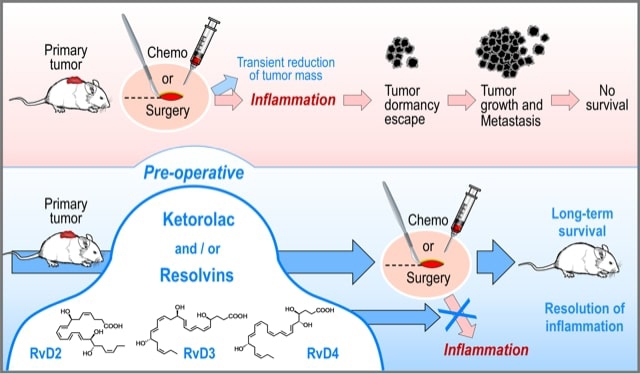
Scientists from UC Davis and Harvard Medical School co-authored the paper on how blocking inflammation and/or activating the resolution of inflammation before surgery or chemotherapy can eradicate small tumors and promote long-term survival in experimental animal cancer models.
The paper, “Preoperative Stimulation of Resolution and Inflammation Blockade Eradicates Micrometastases,” available online beginning June 17, combines the expertise of Professor Bruce Hammock and researcher Jun Yang of UC Davis with that of the Harvard Medical School team led by Dipak Panigrahy and Allison Gartung; Professor Vikas Sukhatme from Emory University School of Medicine, Atlanta; and Professor Charles Serhan from Brigham and Women's Hospital/Harvard Medical School.
“During chemotherapy or surgery, dying cancer cells can trigger inflammation and the growth of microscopic cancerous cells,” said Hammock, a distinguished professor who holds a joint appointment with the UC Davis Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center.


“We found that preoperative, but not postoperative, administration of the nonsteroidal anti-inflammatory drug ketorolac and/or resolvins, a family of specialized pro-resolving autacoid mediators, eliminated micrometastases in multiple tumor-resection models, resulting in long-term survival,” Gartung said. “Moreover, we found that ketorolac and resolvins exhibited synergistic anti-tumor activity and prevented surgery or chemotherapy-induced tumor dormancy escape in our animal models.”
Serhan explained that “Ketorolac unleashed anti-cancer T-cell immunity that was augmented by immune checkpoint blockade, negated by adjuvant chemotherapy, and dependent on inhibition of the COX-1/thromboxane A2 (TXA2) pathway. Pre-operative stimulation of inflammation resolution via resolvins (RvD2, RvD3, and RvD4) inhibited metastases and induced T cell responses.”
“Collectively, our findings suggest a paradigm shift in clinical approaches to resectable cancers," said Sukhatme. "Simultaneously blocking the ensuing pro-inflammatory response and activating endogenous resolution programs before surgery may eliminate micrometastases and reduce tumor recurrence."
This novel approach of blocking inflammation and/or accelerating the resolution of inflammation before a surgical procedure also holds promise for patients who do not have cancer. “More than 30 percent of healthy individuals harbor microscopic cancers," Panigraphy said. "Non-cancer surgery and anesthesia may promote the growth of existing micro-tumors."
Co-authors include:
- Dipak Panigrahy, Allison Gartung, Haixia Yang, Molly M. Gilligan, Megan L. Sulciner, Jaimie Chang, Julia Piwowarski, Anna Fishbein, and DulceSoler-Ferran, all with the Cancer Center, Beth Israel Deaconess Medical Center (BIDMC), Harvard Medical School (HMS);
- Charles N. Serhan from the Center for Experimental Therapeutics and Reperfusion Injury and Department of Anesthesiology, Perioperative and Pain Medicine at Brigham and Women's Hospital, HMS;
- Vikas P. Sukhatme from the Department of Medicine and Center for Affordable Medical Innovation at Emory University School of Medicine;
- Jun Yang and Bruce D. Hammock from the Department of Entomology and Nematology and UC Davis Comprehensive Cancer Center at University of California, Davis;
- Swati S. Bhasin and Manoj Bhasin from the Division of Interdisciplinary Medicine and Biotechnology, Department of Medicine, at BIDMC, HMS;
- Diane R. Bielenberg, Birgitta A. Schmidt and Steven J. Staffa from the Vascular Biology Program, Department of Pathology, and Department of Anesthesiology, Critical Care and Pain Medicine at Boston Children's Hospital (BCH), HMS;
- Matthew A. Sparks from the Division of Nephrology, Department of Medicine at Duke University and Durham VA Medical Centers;
- Vidula Sukhatme from GlobalCures Inc.;
- Mark W. Kieran from Division of Pediatric Oncology at Dana-Farber Cancer Center Institute and Department of Pediatric Hematology/Oncology at BCH, HMS; and Sui Huang from the Institute of Systems Biology.
The researchers said the project drew generous support from the National Cancer Institute (Panigrahy and Serhan), Beth Israel Deaconess Medical Center, the Credit Unions Kids at Heart Team (Panigrahy), C.J. Buckley Pediatric Brain Tumor Fund (Kieran), the Kamen Foundation (Kieran), the Joe Andruzzi Foundation (Kieran), National Institute of Environmental Health Science Superfund Research Program (Hammock); National Institute of Environmental Health Science (Hammock), Sheth family (Sukhatme), Stop and Shop Pediatric Brain Tumor Fund (Kieran), Molly's Magic Wand for Pediatric Brain Tumors (Kieran), the Markoff Foundation Art-In-Giving Foundation (Kieran), and Jared Branfman Sunflowers for Life (Kieran).
For 20 years, the Hammock lab has been researching an inhibitor to an enzyme, epoxide hydrolase, which regulates epoxy fatty acids, but the inhibitor drug was not involved in this particular research. However, many other publications and ongoing cancer research projects are. "My research led to the discovery that many regulatory molecules are controlled as much by degradation and biosynthesis," Hammock said. "The epoxy fatty acids control blood pressure, fibrosis, immunity, tissue growth, depression, pain and inflammation to name a few processes.”
Hammock and colleague Sarjeet Gill, now a distinguished professor at UC Riverside, discovered the target enzyme in mammals while they were postgraduate students at UC Berkeley.

- Author: Kathy Keatley Garvey



Now, newly published research on ovarian cancer, involving an anti-inflammatory compound discovered and developed in the Bruce Hammock lab at the University of California, Davis, and tested at Harvard Medical School on mice models, indicates that the compound not only suppresses inflammation but reduces cancer growth, acting as a “surge protector.”
“We are excited about this research and its potential,” said Hammock, a UC Davis distinguished professor who holds a joint appointment with the Department of Entomology and Nematology and the UC Davis Comprehensive Cancer Center. “Chemotherapy and surgery, the mainstays of conventional cancer treatment, can act as double-edged swords. It is tragic that the very treatments used to cure cancer are helping it to survive and grow.”
The research is a “novel approach to suppressing therapy-induced tumor growth and recurrence,” said the 13-member team from Harvard Medical School/Beth Israel Deaconess Medical Center (BIDMC), UC Davis, Institute of Systems Biology of Seattle, and Emory University School of Medicine of Atlanta.
Their paper, “Suppression of Chemotherapy-induced Cytokine/Lipid Mediator Surge and Ovarian Cancer by a Dual Cox-2, sEH Inhibitor,” appears today in the Proceedings of the National Academy of Sciences (PNAS).
“To prevent tumor-recurrence after therapy, it will be critical to neutralize the inherent tumor-promoting activity of therapy-generated debris,” said lead author Allison Gartung of Harvard Medical School/BIDMC. “Our results indicate that a dual COX-2/sEH inhibitor may offer a novel alternative to protect the body from a debris-mediated inflammatory response.”
Gartung said that the study confirmed that chemotherapy-killed ovarian cancer cells “induce surrounding immune cells called macrophages to release a surge of cytokines and lipid mediators that create an optimal environment for tumors to survive and grow.”
The team treated the mice models with a dual lipid pathway inhibitor discovered several years ago in the Hammock lab. It integrates two anti-inflammatory drugs (COX-2 inhibitor and soluble expoxide hydrolase (sEH) inhibitor) into a single molecule with the aim of reducing tumor angiogenesis and metastasis.
Chemist Sung Hee Hwang of the Hammock lab developed the compound, known as PTUPB, for the study. “The dual inhibitor here follows earlier work we did with it, blocking breast and lung tumors in mice,” Hammock said. “PTUPB is already being clinically evaluated for its therapeutic properties in other diseases.” Chemist Jun Yang of the Hammock lab did the mass spectrometry, showing how stabilization of lipid mediators reduces cancer growth and metastasis.
Lead researcher Dipak Panigrahy, a former Harvard physician turned full-time researcher, described chemotherapy and surgery “as our best tools for front-line cancer therapy, but chemotherapy and surgery create cell debris that can stimulate inflammation, angiogenesis, and metastasis. Thus, the very treatment used by oncologists to try to cure cancer is also helping it survive and grow. Overcoming the dilemma of debris-induced tumor progression is critical if we are to prevent tumor recurrence of treatment-resistance tumors which lead to cancer therapy failure.”
The tumor cell debris generates a “cytokine surge” that can result in a perfect storm for cancer progression. “The dual inhibitor acts as a surge protector,” Panigrahy said.
Panigrahy, who led angiogenesis and cancer animal modeling in the laboratory of Judah Folkman, a leading cancer research laboratory, based the debris model on his mother's chemotherapy treatments, and dedicated the research to his mother and “all other women who lost their lives to ovarian cancer.” American Cancer Society statistics show that among women, ovarian cancer ranks fifth in cancer deaths. A woman's risk of ovarian cancer is about 1 in 78; every year more than 14,000 die from the disease.
“Traditional cancer therapy sets up a dilemma,” Panigrahy commented. “Yes, we need to kill cancer cells but the inevitable byproduct of successfully doing so also stimulates tumor regrowth and progression. The more tumor cells you kill, the more inflammation you create, which can inadvertently stimulate the growth of surviving tumor cells. Overcoming the dilemma of debris-induced tumor progression is paramount if we are to prevent tumor recurrence of treatment-resistant tumors – the major reason for failure of cancer therapy. Our studies potentially pave the path for a new strategy for the prevention and treatment of chemotherapy-induced resistance with potential to translate to the clinic. If successful, this approach may also allow us to reduce the toxic activity of current treatment regimens.”
“The collaborative work in this paper not only defines a common problem with current cancer therapy, but it actually offers a potential solution to reduce metastasis and tumor growth following therapy,” said Primo Lara Jr., director of the UC Davis Comprehensive Cancer Center and associate director of Translational Research. “I am pleased that our Center was involved in this exciting project and we hope we can be involved in translating this basic research to the clinic.”
Panigrahy said that non-steroidal anti-inflammatory drugs (NSAIDs), which include aspirin and ibuprofen, reduce pain, fever and inflammation “bit may have severe side effects including stomach and brain bleeding as well as severe cardiovascular and kidney toxicity. They also do not specifically enhance clearing of debris.”
“We are exploring all options to translate PTUPB to cancer patients especially in combination with current cancer therapies such as chemotherapy, radiation, immunotherapy, or surgery which either directly or indirectly may generate tumor cell debris,” Panigrahy said. “Our next step is to investigate whether our findings are consistent with clinical studies involving human cancer.”
The Hammock lab has been researching the sEH inhibitor for 50 years. As a graduate student at UC Berkeley, Hammock co-discovered the sEH inhibitor with fellow graduate student Sarjeet Gill, now a distinguished professor at UC Riverside.
"We have a series of papers largely in PNAS, with the Panigrahy group showing first our soluble epoxide hydrolase inhibitors block tumor growth and metastasis when used with omega3 fish oils or with COX inhibitors and the role for these compounds in regulating a number of mediators of cancer growth," Hammock said.
Multiple grants funded the research. Hammock, the 31-year director of the UC Davis Superfund Program, received funds the National Cancer Institute and the National Institute on Environmental Health Sciences. The Panigrahy laboratory is funded by the Credit Union Kids at Heart Team. Other grants came from the C. J. Buckley Pediatric Brain Tumor Fund, Molly's Magic Wand for Pediatric Brain Tumors, the Markoff Foundation Art-in-Giving Foundation, the Kamen Foundation, Jared Branfman Sunflowers for Life, and the Joe Andruzzi Foundation. An NIH T32-training grant funded Gartung's work.
The Team
Allison Gartung completed her doctorate at Wayne State University in 2016 and has since served as a postdoctoral research fellow at Harvard Medical School/BIDMC. Highly honored for her work, she won the highest award for a post-doctoral fellow (Santosh Nigam Award) at the 15th International Conference on Bioactive Lipids in Cancer, Inflammation and Related Diseases, held in 2017 in Puerta Vallarta, Mexico. She served as a guest editor of a special double-issue of 24 invited world-experts in Cancer and Metastasis Reviews on Bioactive Lipids.
Dipak Panigrahy was accepted into medical school at Boston University at age 17. He trained in surgery with Dr. Roger Jenkins, who performed the first liver transplant in New England. Over the past decade, Panigrahy led angiogenesis and cancer animal modeling in the Judah Folkman laboratory. He joined the Beth Israel Deaconess Medical Center in 2013, and in 2014 was appointed assistant professor of pathology, and currently has a laboratory in the Center for Vascular Biology Research. Panigrahy is the expert on the team for preclinical tumor models and examining novel concepts for cancer therapy at the preclinical stage –the diversity of models he has created and worked with is unmatched.
Bruce Hammock, UC Davis distinguished professor, is the world expert and discoverer of the dual COX2-sEH inhibitor. He received his doctorate in entomology/toxicology from UC Berkeley and joined the UC Davis faculty in 1980. Highly honored by his peers, Hammock is a fellow of the National Academy of Inventors, which honors academic invention and encourages translations of inventions to benefit society. He is a member of the U.S. National Academy of Sciences, and the recipient of scores of awards, including the Bernard B. Brodie Award in Drug Metabolism, sponsored by the America Society for Pharmacology and Experimental Therapeutics; and the first McGiff Memorial Awardee in Lipid Biochemistry,
Mark Kieran of Bristol-Myers Squibb and Professor Vikas Sukhatme (Dean of Emory School of Medicine), both senior co-authors, are leading world-experts on personalized medicine approaches to support the treatment of cancer patients. Kieran is a leading oncologist with expertise in translating novel therapeutic modalities (beyond chemotherapy/irradiation) into the clinic. Plans for clinical trials involving PTUPB are underway.
Professor Sui Huang, with the Institute for Systems Biology (ISB), is known as the world's leading expert on systems biology and debris-induced tumor growth.

- Author: Kathy Keatley Garvey
Water balloons, water guns, super sprayers, and buckets prevailed when dozens of scientists participated in the 15th annual Bruce Hammock Lab Water Balloon Battle on the Briggs Hall lawn at the University of California, Davis.
The July event, also known as "Bruce's Big Balloon Battle at Briggs," proved to be an international soakfest. That's because the 28 researchers in the Hammock lab hail from seven countries: the United Stares, China, France, Ukraine, Lebanon, Japan and Korea. They include postdoctoral scholars, researchers, graduate students, visiting scholars, visiting graduate students, visiting summer students, short-term visiting scholars and student interns.
The annual battle amounts to 15 minutes, or "15 Minutes of Aim." That's how long it takes for the some 40 water warriors to toss 2,000 water balloons. Joining in were scientists from the Aldrin Gomes lab, UC Davis Department of Neurobiology, Physiology and Behavior; Frank Zalom lab of the UC Davis Department of Entomology and Nematology; and the UC Davis Department of Mathematics, plus family and friends.
Hammock, a UC Davis distinguished professor who holds a joint appointment with the UC Davis Department of Entomology and the UC Davis Comprehensive Cancer Center, hosts the annual event in mid-July when triple-digit temperatures strike the campus. It's an opportunity for the lab members--who work hard throughout the year and play hard for 15 minutes--to engage in a little fun and camaraderie. The thirsty lawn benefits, too.
First the water warriors fill the balloons in an assemblyline procedure, and at exactly 3 p.m., the soakfest begins. As the H2O dwindles, they empty buckets at unsuspecting targets. The last part: picking up every single balloon remnant from the lawn.
Hammock, trained as a entomologist, chemist and toxicologist--and who now focuses his research on human health, is recognized for his work on using natural chemical mediators to control inflammation and intractable pain. He co-discovered the soluble epoxide hydrolase, and many of his more than 1100 publications and patents are on the P450 branch of the arachidonate cascade where the soluble epoxide hydrolase (sEH) degrades natural analgesic and anti-inflammatory compounds.
Hammock, an alumnus of UC Berkeley with a doctorate in entomology, joined the UC Davis faculty in 1980. He is the founding director (1987-present) of the UC Davis NIEHS (National Institute of Environmental Health Sciences) Superfund Research Program and is a founding member (1990-present) of the UC Davis Comprehensive Cancer Center. He has directed the UC Davis NIH/NIEHS Combined Analytical Laboratory for 25 years.
Highly honored by his peers, Hammock is a fellow of the National Academy of Inventors, which honors academic invention and encourages translations of inventions to benefit society. He is a member of the U.S. National Academy of Sciences, a fellow of the Entomological Society of America, and the recipient of the Bernard B. Brodie Award in Drug Metabolism, sponsored by the America Society for Pharmacology and Experimental Therapeutics. He is the first McGiff Memorial Awardee in Lipid Biochemistry. The Eicosanoid Research Foundation recently honored him for work on oxidized lipids.
But on one day in July--for 15 minutes--noted academician Bruce Hammock leaves his Briggs Hall office and transforms into an elite water warrior. He's practiced for 15 years, 15 minutes at a time.
"Bruce has a good aim," said Christophe Morisseau, a Hammock lab researcher who coordinates the annual battles.







- Author: Kathy Keatley Garvey

Titled “The Role of EETs in Pressure-induced Vasoconstriction,” the podcast explains the ground-breaking research involving the role of EETs (Epoxyeicosatrienoic acids) in regulating the myogenic tone in a skeletal muscle small resistance artery. The research, done on rodents, could lead to better control of high blood pressure in humans.
In the podcast, associate editor Mordy Blaustein interviews lead author An Huang (New York Medical College) and expert David Harder (Medical College of Wisconsin) about what Blaustein describes as “an innovative knock-out mouse model, responses of different types of vascular beds to various vasodilatory agents, and the importance of basic studies on SEH inhibitors as the backbone of clinical trials.”
EETs possess cardioprotective properties that are “catalyzed by soluble epoxide hydrolase (sEH) to dihydroxyeicosatrienoic acids (DHETs) that lack vasoactive property,” the seven-member scientific team wrote in their research, Soluble epoxide hydrolase-dependent regulation of myogenic response and blood pressure, published April 15 in the American Journal of Physiology-Heart and Circulatory Physiology.
“To date, the role of sEH in the regulation of myogenic response of resistant arteries, a key player in the control of blood pressure, remains unknown,” they wrote in their abstract. “To this end, experiments were conducted on sEH-knockout (KO) mice, wild-type (WT) mice, and endothelial nitric oxide synthase (eNOS)-KO mice treated with t-TUCB, a sEH inhibitor, for 4 wk. sEH-KO and t-TUCB-treated mice displayed significantly lower blood pressure, associated with significantly increased vascular EETs and ratio of EETs/DHETs. Pressure-diameter relationships were assessed in isolated and cannulated gracilis muscle arterioles. All arterioles constricted in response to increases in transmural pressure from 60 to 140 mmHg. The myogenic constriction was significantly reduced, expressed as an upward shift of pressure-diameter curve, in arterioles of sEH-KO and t-TUCB-treated eNOS-KO mice compared with their controls. Removal of the endothelium, or treatment of the vessels with PPOH, an inhibitor of EET synthase, restored the attenuated pressure-induced constriction to the levels similar to those observed in their controls but had no effects on control vessels. No difference was observed in the myogenic index, or in the vascular expression of eNOS, CYP2C29 (EET synthase), and CYP4A (20-HETE synthase) among these groups of mice. In conclusion, the increased EET bioavailability, as a function of deficiency/inhibition of sEH, potentiates vasodilator responses that counteract pressure-induced vasoconstriction to lower blood pressure.”
Lead author An Huang is with the Department of Physiology, New York Medical College, Valhalla.
In addition to Huang and Hammock, who has a joint appointment with the UC Davis Comprehensive Cancer Center, the co-authors are Sung Hee Hwang of the Hammock lab; Dong Sun, Department of Physiology, New York Medical College, Valhalla; Azita J. Cuevas and Michal L. Schwartzman, both with the Department of Pharmacology, New York Medical College, Valhalla; and Katherine Gotlinger, New York University School of Medicine, Tuxedo.
Grants from the by National Institutes of Health supported the research.



